Functional Medicine for
Adrenal Fatigue & HPA Axis Dysfunction
Beyond Cortisol: The Cumulative Stress Model
and Why Your Body Can’t Keep Up
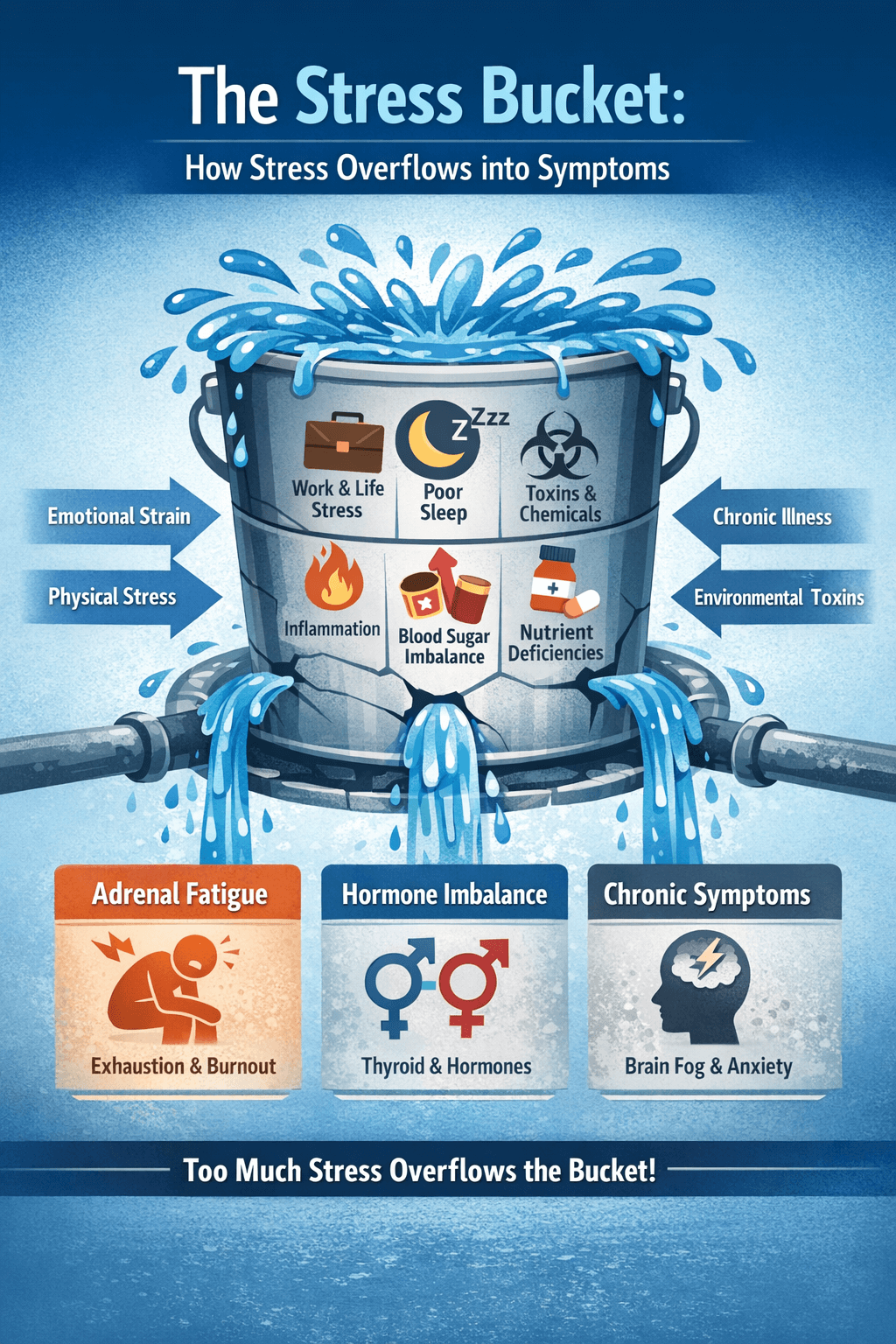
Modern life pushes the human stress response system harder than it was ever designed to handle. Deadlines, lack of sleep, chronic inflammation, environmental toxins, blood sugar swings, emotional trauma, and nutrient depletion all send signals to the same system — the Hypothalamic-Pituitary-Adrenal (HPA) axis, the command center that regulates stress hormones like cortisol.
Over time, this constant demand can leave the body stuck in a cycle of overdrive, imbalance, and eventual exhaustion. Many people call this state adrenal fatigue — a condition where the body struggles to maintain normal energy, focus, mood, sleep, and resilience.
Functional medicine recognizes that adrenal dysfunction is rarely caused by one problem alone. Instead, it reflects the cumulative burden of stressors acting on the body over time, eventually overwhelming the systems that regulate energy, recovery, and hormone balance.

Common Signs and Symptoms of Adrenal fatigue & HPA Axis Dysfunction
-
• Persistent fatigue despite adequate sleep
• Difficulty waking in the morning
• Afternoon energy crashes (2–4 PM)
• Feeling “wired but tired” at night
• Dependence on caffeine to function -
• Brain fog and difficulty concentrating
• Anxiety or feeling overwhelmed
• Irritability or mood swings
• Depression or lack of motivation
• Reduced stress tolerance -
• Trouble falling asleep
• Waking between 1–3 AM
• Light, non-restorative sleep
• Feeling exhausted even after 7–8 hours -
• Blood sugar swings or sugar cravings
• Weight gain around the abdomen
• Hormonal imbalances
• Reduced libido
• Thyroid dysfunction -
• Frequent illness or lowered immunity
• Muscle weakness or body aches
• Salt cravings
• Low blood pressure or dizziness when standing
• Hair thinning or skin changes
• Weight gain - specially around the belly
How Common Is Adrenal Dysfunction?

While the term “adrenal fatigue” is debated in conventional medicine, the underlying concept of chronic stress–related HPA axis dysregulation is well documented in the scientific literature.
Stress and Cortisol Dysregulation Are Extremely Common
Research shows that chronic stress exposure is associated with measurable changes in cortisol patterns and HPA axis signaling.
Key findings include:
• Up to 70–80% of primary care visits are related to stress-associated conditions (American Institute of Stress).
• Chronic stress has been linked to altered cortisol rhythms, reduced resilience, and impaired recovery.
• Studies show that burnout and chronic fatigue conditions frequently involve dysregulated cortisol patterns.
Relevant Research
• McEwen BS. “Protective and damaging effects of stress mediators.” New England Journal of Medicine.
• Chrousos GP. “Stress and disorders of the stress system.” Nature Reviews Endocrinology.
• Clow A et al. “The cortisol awakening response.” Psychoneuroendocrinology.
These studies describe how chronic stress can alter:
• Cortisol rhythms
• HPA axis signaling
• Immune function
• Metabolism
• Brain function
Conventional Medicine vs Functional Medicine: Two Different Views
The Conventional Medical Model
Traditional endocrinology typically recognizes adrenal problems only when the adrenal glands fail in a clear and measurable way. These conditions are relatively rare and include diseases such as:
• Addison’s Disease – when the adrenal glands produce dangerously low levels of cortisol and other adrenal hormones
• Cushing’s Syndrome – when the body produces excessively high levels of cortisol
• Adrenal tumors or structural gland damage
These disorders are typically diagnosed through single blood tests that measure cortisol levels at a specific moment in time.
If cortisol levels fall within the laboratory reference range on that test, the adrenal glands are generally considered “normal.”
However, this approach has an important limitation.
The Functional Medicine Perspective
Functional medicine recognizes that human physiology rarely functions in simple black-and-white categories. Instead, most biological systems exist along a continuum of adaptation and dysfunction.
The adrenal glands are a perfect example of this concept.
In conventional medicine, adrenal disorders are typically only recognized when the glands have reached the extreme end of dysfunction, such as in Addison’s disease (severe adrenal insufficiency) or Cushing’s syndrome (excess cortisol production).
However, long before the adrenal glands reach those extremes, the body often goes through years of stress adaptation and gradual dysregulation of the HPA axis.
During this time, the body is still technically producing cortisol, but the regulation, timing, and signaling of that cortisol can become disrupted.
Functional medicine refers to this pattern as HPA axis dysfunction or adrenal fatigue.
Common Sources of Stress That Affect the Adrenal System
Stress Comes in Many Forms
Another important concept is that the body does not distinguish between different types of stress.
Whether the stress signal comes from the mind, the immune system, the environment, or physical strain, it all feeds into the same biological stress response system.
Many people assume stress refers only to mental or emotional pressure, but the body experiences stress from many different sources.
Physical Stress
• Lack of sleep
• Overtraining or excessive exercise
• Chronic pain or injury
• Surgery or illness
Nutritional Stress
• Blood sugar swings
• Poor diet quality
• Nutrient deficiencies
• Excess caffeine or stimulants
Chemical Stress
• Environmental toxins
• Mold exposure
• Heavy metals
• Medication side effects
• Pesticides and pollutants
Emotional & Psychological Stress
• Work pressure
• Financial stress
• Parenting challenges
• Anxiety or depression
Inflammatory Stress
• Gut inflammation
• Chronic infections
• Autoimmune conditions
• Food sensitivities
Life Event Stress
• marriage
• divorce
• moving
• job changes
• loss of a loved one
• major life uncertainty
The Adrenal System Doesn’t Work Alone
One of the most common mistakes when addressing adrenal fatigue or HPA axis dysfunction is focusing only on cortisol levels or the adrenal glands themselves. While the adrenal glands produce important stress hormones, they do not operate in isolation.
In reality, the adrenal glands are part of a complex communication network involving the brain, hormones, metabolism, immune system, and energy production systems throughout the body. This network is known as the Hypothalamic-Pituitary-Adrenal (HPA) axis, and it constantly responds to signals coming from many different organs and systems.
Because of this interconnected design, adrenal dysfunction is rarely caused by a single problem. Instead, it often reflects imbalances occurring in several other areas of the body that place ongoing demand on the stress response system.
For this reason, simply stimulating the adrenal glands or taking supplements for cortisol alone often fails to solve the deeper issue. To truly restore energy, resilience, and hormone balance, it is important to evaluate the entire system that influences stress regulation.
Key Systems That Influence Adrenal Function
Several major body systems directly affect how the adrenal glands function and how well the body adapts to stress.
-
The thyroid gland regulates the body’s metabolic rate and energy production. When thyroid function slows, the body may compensate by increasing stress signaling through the adrenal system in an attempt to maintain energy levels.
Thyroid dysfunction can therefore contribute to symptoms such as fatigue, brain fog, cold intolerance, and slowed metabolism, while also placing additional strain on the adrenal stress response system.
-
The digestive system and adrenal system are closely connected through immune signaling, inflammation, and the gut-brain axis.
Problems such as:
• intestinal inflammation
• dysbiosis (microbial imbalance)
• food sensitivities
• increased intestinal permeability (“leaky gut”)can trigger immune activation and inflammatory signals that continually stimulate the HPA axis.
Over time, chronic gut stress can significantly contribute to fatigue, mood changes, and hormone disruption.
-
One of cortisol’s primary roles is helping the body maintain stable blood sugar levels.
When blood sugar drops too low, the body releases cortisol and adrenaline to raise glucose levels. If blood sugar fluctuates frequently due to diet, insulin resistance, or metabolic dysfunction, the adrenal system may be repeatedly activated throughout the day.
These constant fluctuations can contribute to symptoms such as:
• energy crashes
• irritability
• sugar cravings
• anxiety or shakiness
• afternoon fatigueStabilizing blood sugar is therefore one of the most important steps in supporting adrenal health.
-
Mitochondria are the tiny energy-producing structures inside every cell of the body. They generate the energy required for brain function, muscle activity, hormone production, and cellular repair.
When mitochondrial function becomes impaired due to inflammation, toxins, nutrient deficiencies, or chronic stress, the body may struggle to produce adequate energy.
This can lead to symptoms commonly associated with adrenal fatigue, including:
• chronic exhaustion
• poor exercise tolerance
• brain fog
• reduced recovery after stressSupporting mitochondrial health is therefore an important component of restoring overall resilience and energy production.
-
Chronic immune activation places constant demand on the stress response system. Conditions such as chronic infections, autoimmune disease, allergies, or systemic inflammation can all stimulate ongoing cortisol signaling.
Over time, this persistent immune stress can contribute to fatigue, hormone disruption, and reduced stress tolerance.
-
The adrenal glands also interact closely with sex hormones such as estrogen, progesterone, and testosterone.
When the body is under chronic stress, resources may shift toward producing stress hormones rather than maintaining balanced sex hormone production. This can contribute to hormonal symptoms such as:
• reduced libido
• menstrual irregularities
• PMS
• mood changes
• reduced vitalityBalancing adrenal health often helps restore healthier hormone signaling across multiple systems.
Because the adrenal system is connected to so many areas of the body, adrenal fatigue is rarely just an adrenal problem. Instead, it often reflects an accumulation of stress signals coming from multiple systems at once, which is why a comprehensive functional medicine approach is often necessary to restore balance.

Why the Body Sometimes Needs Support
Because modern stressors often occur continuously rather than occasionally, many people’s bodies struggle to fully recover between stressful events. Instead of short bursts of stress followed by rest and repair, the stress response system can remain activated for long periods of time.
Over time, this constant demand can begin to disrupt normal biological rhythms, including sleep cycles, hormone balance, immune regulation, and energy production.
Functional medicine does not aim to eliminate stress entirely, because some stress is actually beneficial and necessary for growth, adaptation, and resilience. Healthy stress — such as exercise, learning new skills, or overcoming challenges — helps the body become stronger and more adaptable.
The goal instead is to create measured, balanced stress with adequate recovery.
Just like muscles need recovery after exercise in order to grow stronger, the stress response system also requires periods of restoration to maintain optimal function.
Unfortunately, when stress accumulates from multiple sources — physical, emotional, chemical, inflammatory, and environmental — the body’s ability to recover can become overwhelmed. When this happens, the stress system may remain activated even when there is no immediate threat, leading to persistent fatigue, hormone imbalance, sleep disruption, and reduced resilience.
In many cases, the body simply needs help restoring balance by addressing some of the most common underlying stressors, including:
• improving sleep quality and circadian rhythm regulation
• reducing chronic inflammation
• correcting nutrient deficiencies that affect energy production and hormone signaling
• supporting hormone balance, including thyroid and sex hormones
• improving gut health and digestion, which strongly influence stress signaling
• reducing toxin exposure and improving detoxification pathways
• stabilizing blood sugar regulation
• addressing lifestyle and emotional stress patterns
When these underlying stressors are identified and corrected, the body often regains its ability to adapt to stress more effectively and maintain stable energy levels throughout the day.
Rather than simply masking fatigue or pushing the body harder with stimulants, functional medicine focuses on restoring the body’s natural resilience and recovery capacity, allowing the stress response system to function the way it was designed.
Other recommended reading:
