Functional Medicine for
SIBO(Small Intestine Bacterial Overgrowth)
Breaking the Cycle of Recurring SIBO &
Restoring Balance to the Small Intestine

You eat a meal and within hours you’re bloated, gassy, and uncomfortable. Sometimes it’s diarrhea, other times constipation. You try to eat “clean,” take probiotics, or even do a round of antibiotics — yet the symptoms return again and again.
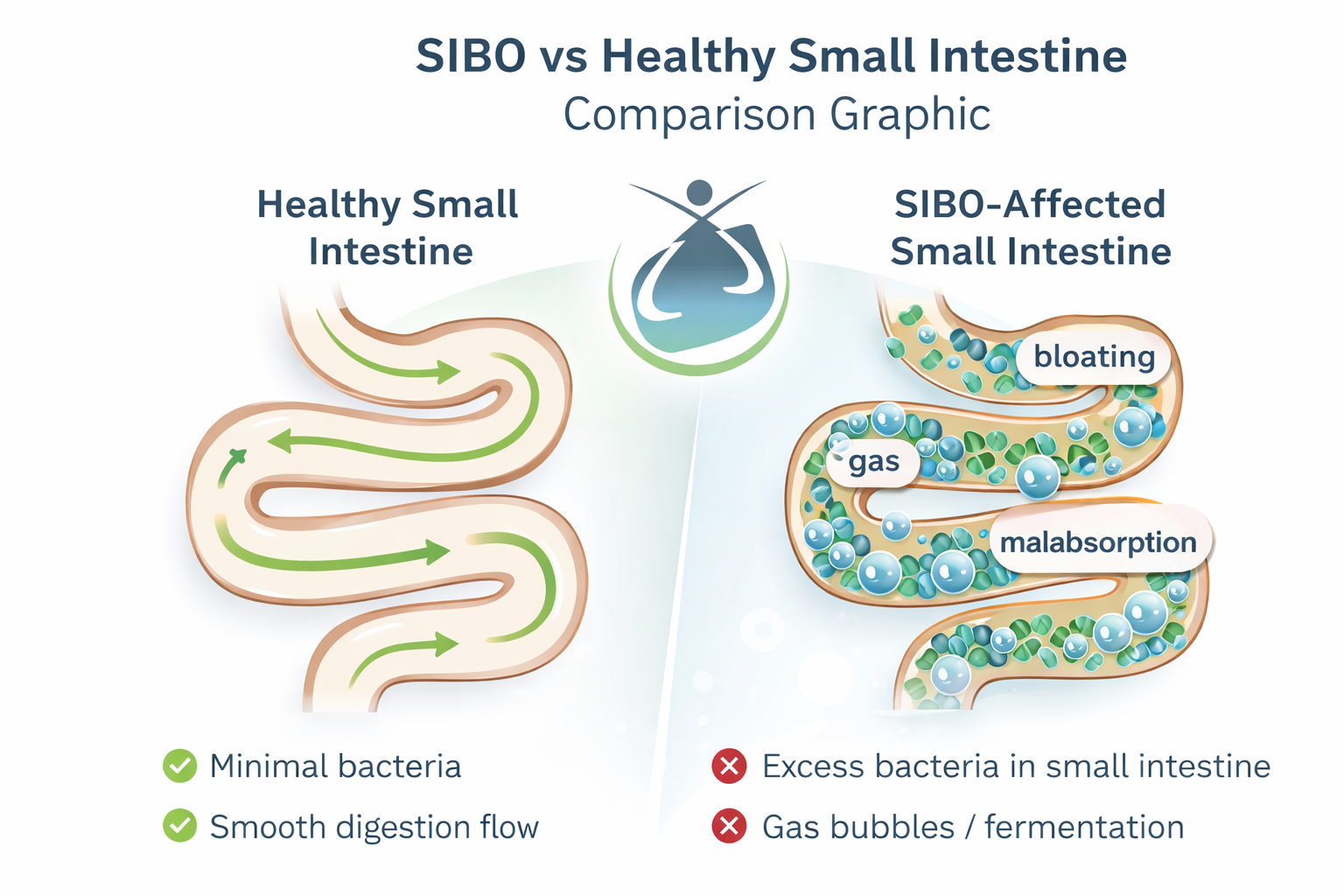
This is the frustrating reality for many people with Small Intestinal Bacterial Overgrowth (SIBO). It’s not just “bad digestion” or something you ate. It’s a sign that the delicate ecosystem in your small intestine has been thrown off balance, and the underlying reasons keeping it that way have not yet been addressed. Small Intestine Bacterial Overgrowth (SIBO), a condition where bacteria that belong in your large intestine migrate and multiply in the small intestine.
At Premier Integrative Functional Medicine, we see SIBO patients every week who feel trapped in this recurring cycle. The good news is that functional medicine offers a clear path to break that cycle by identifying why the overgrowth keep happening and correcting the root causes — not just temporarily reducing the bacteria.
Many patients come to us after years of being told “it’s just IBS.” Functional medicine changes the story from symptom management to true restoration of balance.
Gut Health Is the Foundation of Whole-Body Health
“Nearly 70% of your immune system lives in your gut, and the gut is directly connected to your brain, hormones, inflammation levels, and detoxification pathways. When the gut is out of balance — as it is with SIBO — it can trigger symptoms far beyond digestion, affecting energy, mood, skin, immunity, and mental clarity.”
This is why simply killing off excess bacteria is rarely enough. True healing requires restoring proper gut function and addressing the deeper imbalances that allowed SIBO to develop in the first place.
SIBO Is Far More Common Than Most Realize - And Recurrence is the Real Problem
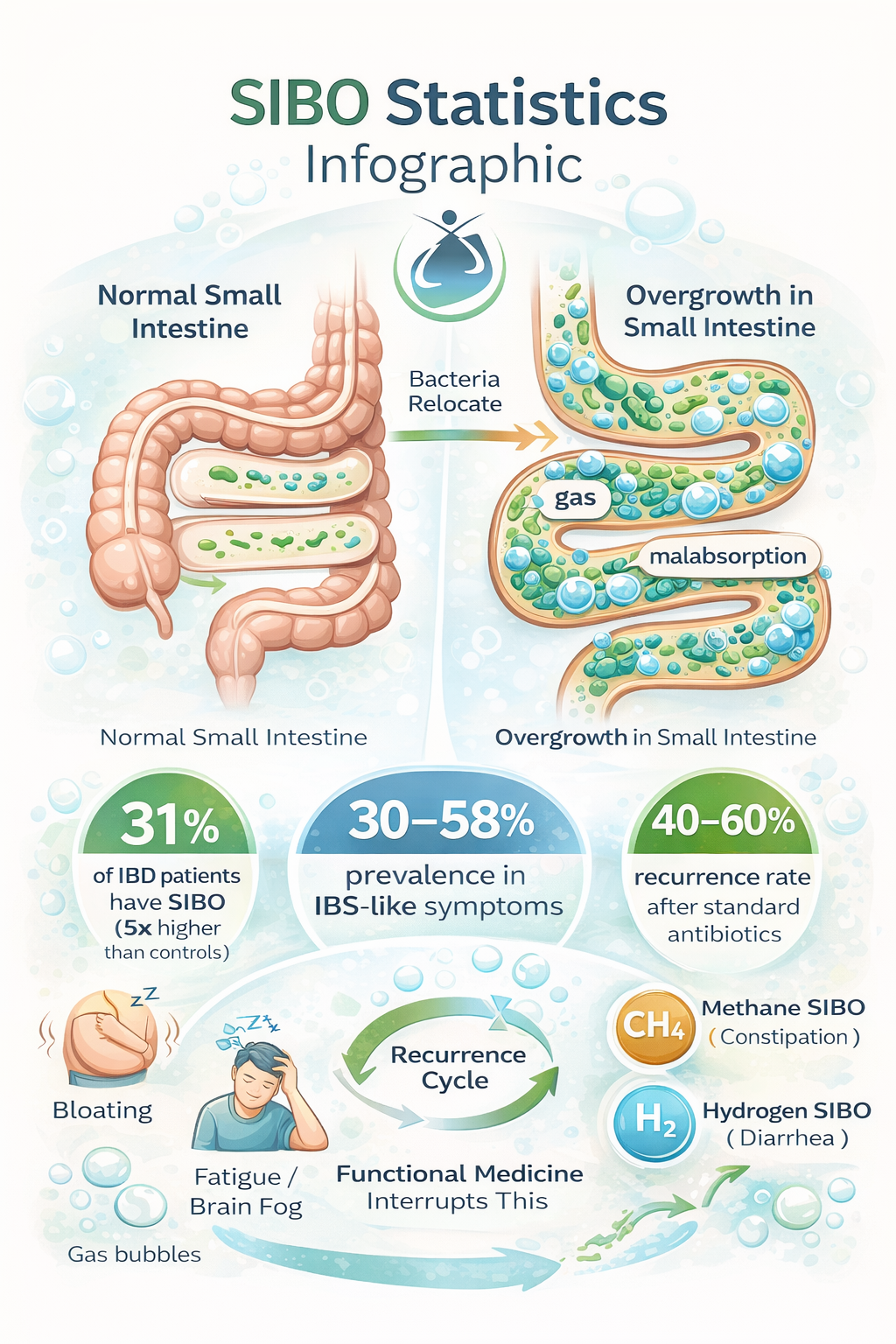
Up to 31% of patients with inflammatory bowel disease (IBD) test positive for SIBO — 5 times higher than healthy controls.
In people with IBS-like symptoms, prevalence ranges from 30–58%depending on the diagnostic test used.
Recurrence rates after standard antibiotic treatment can reach 40–60% within 9–12 months — because antibiotics alone rarely fix the underlying motility or barrier issues.
Surprising Facts Most People Don’t Know
SIBO is not an “infection” — it’s an overgrowth of the normal bacteria that belong in your colon. The problem is location and quantity, not the type of bug.
It can cause B12 deficiency even if you eat plenty of meat — leading to fatigue, brain fog, or even tingling in your hands and feet.
Post-viral illnesses (including COVID) have been linked to a measurable rise in new SIBO cases due to temporary motility slowdown.
Methane-dominant SIBO (often called IMO) is strongly tied to constipation, while hydrogen-dominant tends to cause diarrhea — that’s why one-size-fits-all treatments fail so often.
Why Is SIBO More Common Now?
Our modern world has created several perfect conditions for SIBO to thrive. Widespread use of acid-suppressing medications (PPIs), frequent courses of antibiotics, diets high in processed foods and low in fiber, chronic stress that slows intestinal motility, and sedentary lifestyles that reduce the gut’s natural “housekeeping waves” all contribute to the rise in cases.
Common Symptoms of SIBO
The symptoms of SIBO are often vague and overlap with IBS, food sensitivities, or even stress - which is why so many people go undiagnosed for years.
Digestive Symptoms
Persistent bloating (often worse after eating)
Gas and abdominal distention
Diarrhea, constipation, or alternating between both
Food sensitivities (especially to carbs/FODMAPs)
Systemic Symptoms
Brain fog or difficulty concentrating
Chronic fatigue
Nutrient deficiencies
Unexplained weight changes
Often Overlooked Signs
Acne, eczema, or skin flare-ups
Hormonal imbalances
Anxiety or mood changes
Bad breath (halitosis)
Different Types of SIBO
Hydrogen-dominant SIBO – Typically causes diarrhea, bloating, and urgency
Methane-dominant SIBO (IMO) – Often linked to constipation and slower motility
Hydrogen Sulfide SIBO – Associated with very foul-smelling gas, diarrhea, and sometimes neurological symptoms
Root Causes and Triggers of SIBO
SIBO rarely develops without underlying issues that impair normal gut function. The most frequent drivers we see include impaired migrating motor complex (the gut’s natural housekeeping wave), low stomach acid (often from long-term PPI use), adhesions or scar tissue from surgery or endometriosis, chronic stress and vagus nerve dysfunction, structural problems like ileocecal valve dysfunction, hypothyroidism or other hormonal imbalances, and previous gastrointestinal infections or food poisoning.
Why Functional Medicine & What It Can Do for SIBO
Why Conventional Antibiotics Often Fall Short — And How Functional Medicine Breaks the Cycle
Standard care usually means a 2-week course of rifaximin. While it can reduce bacterial load short-term, it doesn’t address why the bacteria overgrew in the first place (slow migrating motor complex, low stomach acid, adhesions, etc.). That’s why relapse is so common.
At Premier IFM we use a root-cause, 5R framework:
Remove — targeted antimicrobials (herbal or pharmaceutical)
Replace — digestive enzymes, bile support, and stomach acid if needed
Repair — heal the intestinal lining with nutrients like glutamine and zinc
Reinoculate — strategic probiotics and prebiotics (only after overgrowth is cleared)
Rebalance — restore motility with prokinetics, stress management, and personalized nutrition
Results our patients typically see:
Dramatic reduction in bloating starting within 4–6 weeks - however, this entire process does take time
Normalized bowel habits
Sustained energy and better nutrient absorption
Recurrence rates under 10% when root causes are fully addressed (versus 40–60% with antibiotics alone)
We also offer advanced breath testing (lactulose/glucose) right in our Placentia office so you get answers fast.
Section: SIBO vs IBS – What’s the Difference?
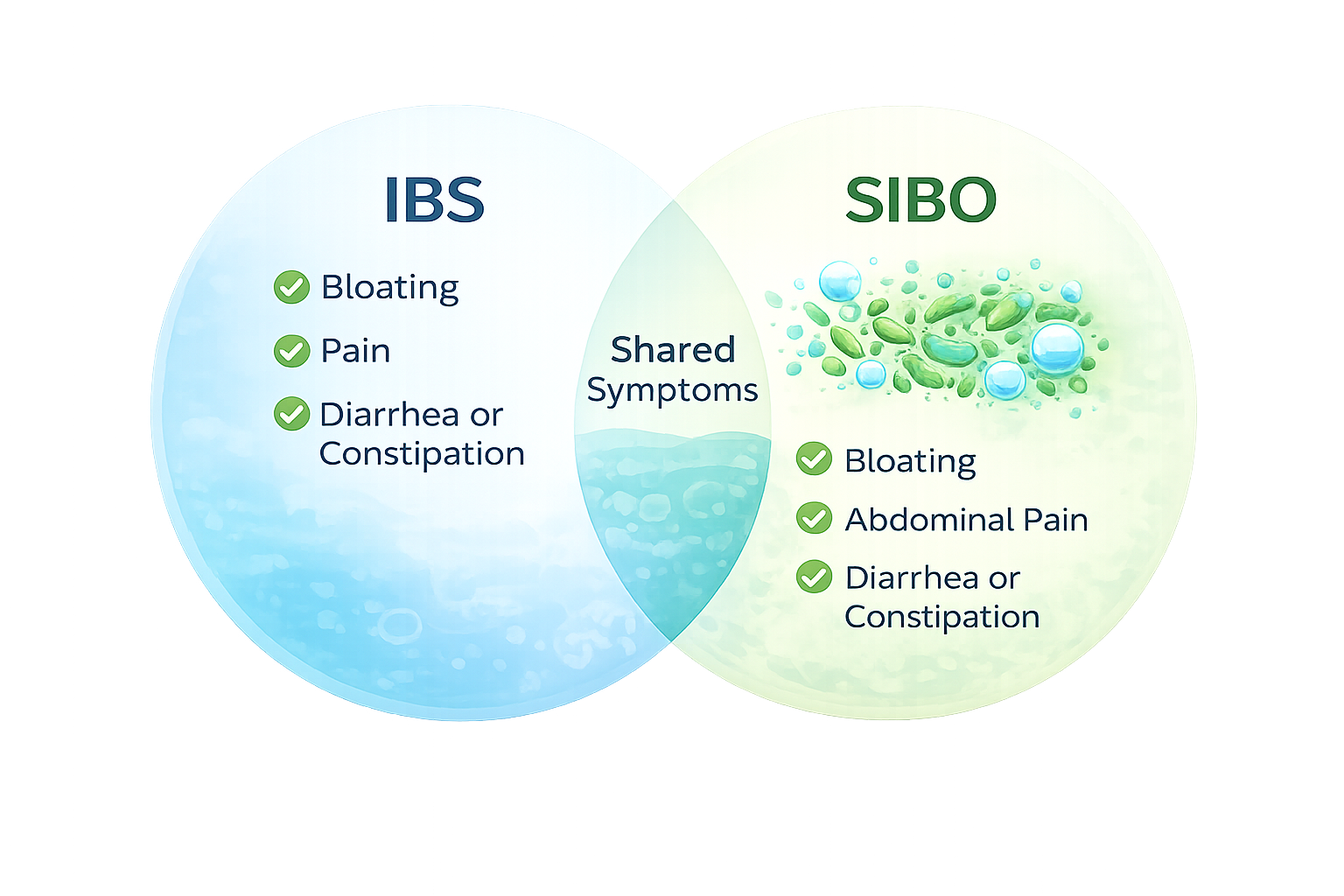
SIBO and IBS (Irritable Bowel Syndrome) are often confused—and for good reason. They share many of the same symptoms, but they are not the same condition.
The Key Difference
IBS is a diagnosis based on symptoms
SIBO is a specific underlying cause (bacterial overgrowth in the small intestine)
In fact, research shows that a large percentage of people diagnosed with IBS may actually have SIBO.
SIBO vs. IBS Comparison
SIBO
Caused by bacterial overgrowth in the small intestine
can be confirmed with breath testing
Often linked to root causes like poor motility or low stomach acid
Treatable by addressing the underlying imbalance
IBS
Functional disorder with no single identified cause
Diagnosed based on symptoms (Rome IV criteria)
Often labeled when no clear cause is found
Typically managed with symptom control
Why This Matters
Many patients are told they have IBS and are given general advice—but never tested for SIBO.
If SIBO is the root cause, treating IBS alone won’t resolve symptoms long-term.
Functional Medicine Insight
At Premier IFM, we look beyond the IBS label to identify whether SIBO—or another root cause—is driving your symptoms.
This allows us to move from symptom management to true resolution.
What Helps: Foods That Support Symptom Relief
These lower-fermentable, easier-to-digest foods reduce the substrate available for bacterial fermentation in the small intestine, often leading to less gas, bloating, and abdominal distension.
Proteins (generally well-tolerated):
Eggs, chicken, turkey, beef, fish, and seafood (plain, unprocessed)
Firm tofu or tempeh (in moderation)
Vegetables (low-FODMAP options):
Carrots, cucumbers, zucchini, spinach, lettuce, tomatoes, eggplant, green beans, bok choy, potatoes (white or sweet in moderation)
Broccoli heads (small portions, < ¾ cup)
Fruits (limited portions):
Strawberries, blueberries, grapes, oranges, kiwi, pineapple, cantaloupe
Grains & Starches:
White rice, quinoa, oats, rice cakes, gluten-free crackers or pasta (corn- or rice-based), corn flakes
Dairy & Alternatives:
Hard cheeses (cheddar, feta, brie, camembert), lactose-free milk, almond milk (unsweetened), soy milk (limited)
Other Helpful Choices:
Eggs, olive oil, herbs like basil or parsley (instead of garlic/onion), dark chocolate (small amounts), maple syrup or table sugar (in very small quantities)
Bonus Tip from Our Approach: Spacing meals 4–5 hours apart supports the Migrating Motor Complex (MMC), your gut’s natural “housekeeping” wave that helps clear bacteria from the small intestine. Many patients also benefit from gentle prokinetic support (herbal or medication) alongside these foods.






What Doesn’t Help (Foods That Often Worsen Symptoms)
These foods are high in fermentable carbohydrates (FODMAPs) or other compounds that bacteria in the small intestine can rapidly ferment, producing gas and triggering bloating, pain, and irregular bowels.
High-FODMAP Foods to Limit or Avoid (Especially During Active Symptoms or Treatment):
Vegetables: Onions, garlic, asparagus, cauliflower, mushrooms, peas, artichokes, Brussels sprouts
Fruits: Apples, pears, cherries, peaches, watermelon, dried fruits, high-fructose items (honey, agave)
Grains & Legumes: Wheat-based products (bread, pasta, cereal), barley, rye, beans, lentils, chickpeas
Dairy: Regular milk, yogurt, soft cheeses, ice cream (due to lactose)
Sweeteners & Additives: Sugar alcohols (sorbitol, mannitol, xylitol in sugar-free gum/mints), high-fructose corn syrup, sucralose
Other Common Triggers:
Highly processed or sugary foods
Large amounts of raw fibrous vegetables or beans
Fermented foods (sauerkraut, kimchi, kefir) during active overgrowth phases — these can be reintroduced later for microbiome support
Alcohol and carbonated drinks (they can irritate and add gas)
Surprising Fact: Even “healthy” foods like garlic, onions, and legumes — excellent for colon health in most people — can significantly worsen SIBO symptoms because the bacteria ferment them too early in the digestive tract.
How We Use Diet at Premier IFM
At Premier Integrative Functional Medicine, we customize the dietary approach for each SIBO patient rather than using a one-size-fits-all plan. Depending on your symptoms, test results, and any co-existing issues (such as candida overgrowth or severe dysbiosis), we typically recommend either a short-term low-FODMAP diet or an Anti-Candida diet.
Short-term low-FODMAP phase (usually 2–6 weeks) to quickly reduce fermentable carbohydrates that feed bacterial overgrowth in the small intestine, providing rapid relief from bloating, gas, and abdominal discomfort.
Anti-Candida diet when testing or symptoms suggest concurrent yeast overgrowth. This approach limits sugars, refined carbohydrates, and certain fermented foods while emphasizing vegetables, quality proteins, and healthy fats to help restore microbial balance.
Phased reintroduction of foods after the initial restrictive phase. This careful process helps identify your personal triggers and safely expands your food choices without triggering a return of symptoms.
Transition to a balanced, anti-inflammatory diet / detox diet focused on whole foods, adequate protein, healthy fats, and a gradual, well-tolerated increase in fiber to support healthy gut motility and help prevent recurrence.
For severe or stubborn cases, we may discuss a temporary elemental diet (a predigested liquid nutrition formula) under close supervision. This approach has been shown to significantly reduce bacterial load in a short period while giving the gut a chance to rest and heal.
Our goal is never long-term restriction or elimination. Instead, we use diet strategically as a therapeutic tool — creating a clear window for healing the gut, reducing overgrowth, and then building a sustainable, nourishing way of eating that supports long-term balance and keeps SIBO from returning.
Frequently Asked Questions
-
SIBO is typically caused by impaired gut motility, low stomach acid, or disruptions to the gut microbiome that allow bacteria to accumulate in the small intestine.
-
In most cases, no. Without addressing the root cause, symptoms tend to persist or return.
-
SIBO is commonly diagnosed using a breath test that measures hydrogen and methane gas levels after consuming a specific substrate.
-
There isn’t a true “quick fix” for SIBO—but that’s actually a good thing. SIBO develops over time due to underlying imbalances, so lasting relief comes from addressing the root cause, not just temporarily reducing symptoms.
The most effective approach combines a targeted antimicrobal regimen to reduce bacterial overgrowth with support for digestion, gut motility, and long-term balance. When done correctly, this leads to more sustainable results—not just short-term relief.
-
Recurrence happens when the root issue—such as slow gut motility or digestive dysfunction—is not corrected.
-
Diet can play a powerful role in reducing symptoms, but it rarely eliminates SIBO on its own.
While dietary changes (like low FODMAP or SIBO-specific diets) can help decrease fermentation and provide relief, they don’t address the underlying bacterial overgrowth.
For lasting results, a comprehensive approach is typically needed—one that includes targeted antimicrobials, support for gut motility, and strategies to repair and restore proper digestive function.
Additional Recommended Reading:
