Functional Medicine for
Diabetes, Obesity, and Metabolic Dysfunction
When Diet and Medications Aren’t Enough,
It’s Time to Address the Root Causes of Metabolic Dysfunction
Are you tired of chasing blood sugar numbers with endless pills, strict diets that don't last, or the frustration of weight that won't budge—no matter how hard you try? You're not alone. Millions struggle with type 2 diabetes, prediabetes, insulin resistance, and obesity, feeling like their body is working against them. Conventional approaches often manage symptoms... but they rarely fix what's really broken.
At Premier Integrative & Functional Medicine, we believe true healing starts by asking: Why is your body no longer responding to insulin? What hidden triggers—gut imbalances, chronic inflammation, hormone disruptions, nutrient gaps, stress overload, or environmental toxins—are driving this metabolic chaos?
Our functional medicine approach goes beyond surface-level fixes. We uncover and address the root causes of metabolic dysfunction through personalized testing, targeted nutrition strategies, gut health restoration, stress & hormone optimization, sleep support, and lifestyle changes tailored to you. Many patients discover they can improve insulin sensitivity, stabilize blood sugar naturally, regain energy, shed stubborn weight, and even move toward reversing type 2 diabetes—without relying solely on medications.
If you're ready to stop just "managing" your condition and start restoring your body's natural balance for lasting metabolic health, you're in the right place.
Take the first step toward feeling like yourself again—explore how we help patients reclaim their vitality every day.




Signs and Symptoms of Diabetes and Metabolic Dysfunction
Diabetes and metabolic dysfunction can develop gradually, and many people may experience symptoms long before receiving a diagnosis. In fact, individuals with prediabetes or insulin resistance may have subtle signs that often go unnoticed.
Common Early Symptoms
Some of the most well-known symptoms of diabetes include:
Increased thirst
Frequent urination
Fatigue or low energy
Blurred vision
Increased hunger
These symptoms are often related to elevated blood sugar levels and changes in how the body processes glucose.
Additional Signs That Are Often Overlooked
Beyond the classic symptoms, metabolic dysfunction can affect multiple systems in the body. Some individuals may experience:
Numbness or tingling in the hands and feet (neuropathy)
Frequent infections (including bacterial or yeast infections)
Slow wound healing
Dry or irritated skin
Unexplained weight changes
Because these symptoms are not always immediately associated with blood sugar issues, many people may not realize they are related to underlying metabolic imbalance.
Long-Term Health Effects of Uncontrolled Diabetes
Over time, chronically elevated blood sugar levels can affect blood vessels, nerves, and organ systems.
According to the CDC, diabetes is associated with an increased risk of:
High blood pressure
Nerve damage (neuropathy)
Kidney disease
Vision problems
Stroke
These complications typically develop gradually and are often influenced by how well blood sugar and overall metabolic health are managed.
Understanding Blood Sugar and Energy
Glucose is the body’s primary source of energy. When blood sugar is not properly regulated, cells may not receive the energy they need efficiently, which can contribute to symptoms such as:
Difficulty concentrating
Fluctuating energy levels
This is often related to insulin resistance, where the body’s cells do not respond effectively to insulin.
How Diabetes Is Diagnosed
Diabetes is typically diagnosed through blood testing. Common tests include:
Fasting blood glucose
Oral glucose tolerance test (OGTT)
Hemoglobin A1C (HbA1c)
The HbA1c test reflects average blood sugar levels over approximately the past 2–3 months and is widely used to assess long-term glucose control.
Functional Lab Testing for Metabolic Health
Common tests may include:
Hemoglobin A1C (HbA1c) – reflects average blood sugar over 2–3 months
Fasting insulin – helps assess insulin resistance
Fasting glucose – measures current blood sugar levels
Lipid panel – evaluates cholesterol and cardiovascular risk
Inflammatory markers – help assess underlying inflammation
These markers can help guide a more personalized and effective treatment plan.
What Causes Diabetes and Metabolic Dysfunction?
Diabetes is often thought of as a condition caused simply by poor diet or excess weight—but in reality, it is far more complex.
While nutrition and body composition can play a role, many patients are surprised to learn that metabolic dysfunction can develop even in individuals who appear otherwise healthy. It is not uncommon for someone to feel relatively well, maintain a normal weight, and still show signs of insulin resistance or prediabetes on lab testing.
Diabetes does not happen overnight—it develops over time. Reversing diabetes ALSO takes time and does not happen overnight.
It is the result of underlying imbalances in how the body regulates blood sugar, processes nutrients, and responds to insulin.
A Progressive Condition, Not a Sudden Diagnosis
Rather than something you “catch,” type 2 diabetes typically develops gradually through a process that may include:
Insulin resistance
Blood sugar dysregulation
Metabolic stress
Chronic low-grade inflammation
In many cases, these changes begin years—sometimes decades—before a diagnosis is made.
This is a lifestyle that takes a lifestyle change.
Why This Matters
Because diabetes develops over time, there is often a window of opportunity to identify early changes and address contributing factors.
Many individuals who are diagnosed with prediabetes or type 2 diabetes may have underlying drivers that go beyond just diet and weight, including:
Chronic stress
Poor sleep
Hormonal imbalances
Inflammation
Environmental exposures
Genetic predisposition
Understanding these contributing factors is key to taking a more comprehensive approach to metabolic health.
A Functional Medicine Perspective
At Premier Integrative & Functional Medicine, we recognize that diabetes is rarely caused by a single factor. Instead, it is typically the result of multiple systems in the body becoming dysregulated over time.
By identifying and addressing these underlying contributors, it may be possible to improve metabolic function and support better long-term health outcomes.
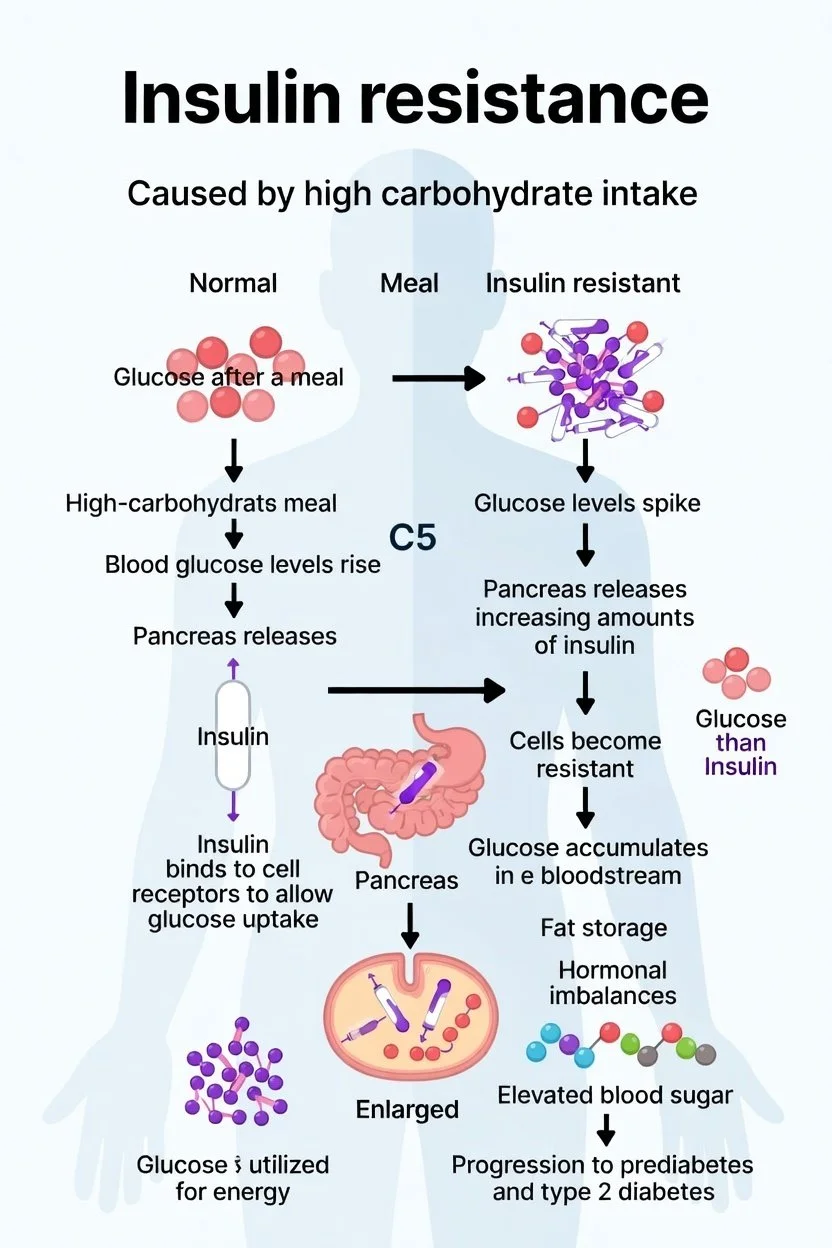
What Is Insulin Resistance?
Insulin resistance occurs when the body’s cells no longer respond effectively to insulin, a hormone that helps regulate blood sugar levels. As a result, the body must produce more insulin to keep blood sugar stable.
Over time, this can lead to:
Elevated blood sugar
Increased fat storage
Hormonal imbalance
Progression toward prediabetes and type 2 diabetes
Insulin resistance is considered one of the primary drivers of metabolic dysfunction and often develops years before a formal diagnosis is made.
Root Causes of Diabetes and Metabolic Dysfunction
From a functional medicine perspective, diabetes is rarely caused by a single factor. Instead, it is typically the result of multiple underlying imbalances that affect how the body regulates blood sugar and metabolism.
Chronic high sugar and processed food intake
Insulin resistance
Chronic stress and cortisol imbalance
Poor sleep quality
Gut health imbalances
Chronic inflammation
Environmental toxins
Sedentary lifestyle
Understanding these root causes allows for a more targeted and personalized approach to care.
Early Warning Signs of Metabolic Dysfunction
Metabolic dysfunction often develops gradually, with early symptoms appearing long before a diagnosis is made.
Common early signs may include:
Fatigue, especially after meals
Sugar cravings
Brain fog or difficulty concentrating
Weight gain around the midsection
Difficulty losing weight
Energy crashes throughout the day
Elevated fasting blood sugar
Recognizing these signs early may provide an opportunity to address underlying imbalances before they progress.
The Functional Medicine Approach to Metabolic Health
At Premier Integrative & Functional Medicine, we take a personalized, root-cause approach to diabetes and metabolic dysfunction.
Rather than focusing only on blood sugar levels, we work to improve:
Insulin sensitivity
Blood sugar regulation
Metabolic flexibility (the body’s ability to switch between fuel sources)
This approach may include:
Targeted nutrition strategies
Gut health optimization
Stress and hormone regulation
Sleep improvement
Personalized supplementation when appropriate
Our goal is to support the body’s ability to restore balance and function more efficiently over time.

Lifestyle Factors That Influence Blood Sugar
Lifestyle factors play a critical role in blood sugar regulation, insulin sensitivity, and overall metabolic health. Nutrition patterns, food quality, sleep duration, stress levels, physical activity, and meal timing all directly influence how the body processes glucose and maintains stable energy levels. Poor sleep, chronic stress, sedentary behavior, and diets high in processed foods have all been associated with impaired blood sugar control and insulin resistance. By improving these key lifestyle factors, individuals may support better metabolic function and reduce the risk of developing prediabetes or type 2 diabetes over time.
Common Questions about Diabetes and Metabolic Health
-
In many cases, insulin resistance can be improved through targeted lifestyle and medical interventions, especially when addressed early.
-
Prediabetes refers to elevated blood sugar levels that are not yet high enough for a diabetes diagnosis, while diabetes involves consistently elevated blood sugar levels that meet diagnostic criteria. Commonly you will inflammation markers starting to rise as well with prediabetes.
-
Yes. Many individuals with prediabetes or early-stage type 2 diabetes may have mild or no symptoms, which is why testing is important.
-
Metabolic syndrome is a group of conditions—including high blood sugar, increased abdominal fat, high blood pressure, and abnormal cholesterol levels—that increase the risk of diabetes and cardiovascular disease.
Case in point: Patient “J”

I recently worked with a fit, late-thirties male patient (let's call him J) who had always been active and healthy. Recently married and planning a family, he was unexpectedly feeling run down, fatigued, and unwell despite maintaining 3–4 hours of exercise weekly and not being overweight.
After a detailed history, several clues emerged, including recent home renovations on a 'fixer-upper' property where he'd been heavily using Roundup to clear weeds in the yard. Lab results were eye-opening: his HbA1c was 6.5, in the diabetic range.
We explored potential environmental factors, including glyphosate exposure from Roundup, which research suggests can disrupt gut microbiome balance and contribute to metabolic issues like insulin resistance in some contexts. While not the only factor, this aligned with his symptoms and history.
Our plan focused on removing potential toxins (starting with discontinuing Roundup and minimizing other exposures), implementing an 8-week targeted detox protocol, optimizing nutrition, supporting gut health, and continuing his exercise routine. Over time, J's energy improved dramatically, his follow-up labs showed normalized blood sugar control, and he and his wife welcomed a healthy baby boy.
This case reminds us how addressing root causes—beyond just blood sugar numbers—can lead to meaningful restoration of metabolic health.
