Functional Medicine for
Insomnia & Sleep Disorders
Why Sleeping Pills Don’t Fix the Problem -
Symptom suppression vs correction

Struggling to Fall Asleep or Waking Up at 2 or 3 AM Night After Night?
Struggling to fall asleep, waking up in the middle of the night, or feeling exhausted no matter how many hours you spend in bed can be incredibly frustrating.
You’re not alone — you are not the problem. It’s not just “stress” or “getting older.”
Chronic loss of sleep can leave you feeling exhausted yet wired, lying awake for hours or jolting awake in the early morning hours, unable to fall back asleep. It is often the same frustrating cycle: tossing and turning at bedtime, waking up around 2 or 3 AM with a racing mind or a jolt of anxiety, and then dragging through the day with brain fog, irritability, and crushing fatigue.
Insomnia and sleep disorders not isolated issues, they are signals from your body that something deeper is out of balance. Whether it’s disrupted cortisol rhythms, hormone fluctuations, blood sugar instability, gut inflammation, or a dysregulated nervous system, your sleepless nights are your body’s way of asking for help.
At Premier Integrative Functional Medicine, we don’t reach for another sleeping pill that simply masks the symptoms. Instead, we listen to what your sleep is trying to tell us, identify the root causes, and gently guide your body back into natural, deep, restorative sleep — so you can finally wake up feeling refreshed and energized.
Sleep Is the Barometer of Your Overall Health
Sleep does not exist in isolation. It is deeply interconnected with nearly every major system in the body.
When sleep is disrupted, we often see parallel dysfunction in:
Poor sleep raises cortisol, which in turn disrupts blood sugar regulation and promotes inflammation. Elevated inflammation can impair gut health and hormone conversion, while blood sugar instability and gut issues can further disturb sleep. It quickly becomes a self-reinforcing cycle.
This is why many people with chronic insomnia also experience fatigue, weight gain, anxiety, digestive problems, brain fog, low libido, or even autoimmune symptoms. Sleep is not separate from these conditions — it is intertwined with them.
Research supports this bidirectional relationship: poor sleep quality is linked to increased systemic inflammation and altered cortisol patterns, while inflammation and metabolic imbalances can make restorative sleep more difficult to achieve.
When sleep improves, many other systems often begin to stabilize — and the reverse is also true. Addressing the root causes that affect your sleep frequently leads to improvements across multiple areas of health.


Why Sleeping Pills Often Provide Only Temporary Relief
We understand how tempting sleeping pills can feel when you’re exhausted and desperate for rest. Many people turn to them hoping for a quick solution to sleepless nights. While they can help you fall asleep faster in the short term, their benefits are usually limited — and they come with real risks that become more concerning with ongoing use.
Research shows that tolerance can develop quickly, often within days to a few weeks, meaning the medication loses effectiveness over time. When people try to stop, they frequently experience rebound insomnia — where symptoms return even stronger than before, sometimes for days or weeks.
Common side effects include next-day grogginess, daytime sedation, dizziness, and impaired coordination. These residual “hangover” effects can increase the risk of falls, fractures, and car accidents — particularly in older adults. Long-term use has also been associated with cognitive concerns, including memory issues and, in some studies, a higher risk of dementia.
What sleeping pills don’t do is equally important:
They don’t fix disrupted cortisol rhythms that keep you wired at night and tired during the day.
They don’t balance blood sugar swings that can cause middle-of-the-night awakenings.
They don’t address underlying hormone imbalances (such as thyroid, progesterone, or melatonin issues).
They don’t improve true sleep architecture — the natural cycles of deep restorative sleep and REM that your body needs for repair and recovery.

Sedation is not the same as restorative sleep.
Many patients tell us they can “knock themselves out” with medication, but they still wake up feeling unrefreshed, foggy, and drained. That’s because sleeping pills primarily sedate the brain rather than supporting the deep, quality sleep your body needs to restore energy, clear toxins, and regulate mood and hormones.
At Premier Integrative Functional Medicine, we believe it’s important to look beyond temporary symptom suppression. By identifying and gently correcting the underlying imbalances driving your sleep issues, we help many patients achieve natural, refreshing sleep that lasts — without relying on medications long-term.
Sleep Adapts — And That’s the Problem
One of the most frustrating aspects of insomnia is how quickly the body adapts.
A supplement works for a few weeks… then it stops.
A medication helps for a while… then the dose needs to increase.
Something that once worked no longer does.
This happens because your nervous system is highly efficient at adapting. When sleep is artificially induced — whether by medication or supplements — without addressing the underlying imbalance, the body compensates and finds ways around it.
This is a discouraging a cycle:
Try something → It works temporarily → It stops working → Try something new → Repeat.
Over time, many people start to believe their sleep is simply “broken” or that they’ll never sleep normally again.
In reality, your body is doing exactly what it’s designed to do — adapt. Until the root physiologic stressors (such as cortisol rhythms, hormone imbalances, blood sugar swings, or gut issues) are properly addressed, this cycle of temporary relief followed by disappointment tends to continue.

Sleep Statistics & Surprising Facts
Sleep Problems Are Far More Common Than Most People Realize
If you’re struggling with insomnia or poor sleep, know that you’re definitely not alone. Sleep disorders have become one of the most widespread health challenges today.
Approximately 1 in 3 adults in the United States reports symptoms of insomnia.
About 10–15% of adults suffer from chronic insomnia, meaning they experience symptoms at least three nights per week for three months or longer.
Nearly 40% of adults report difficulty falling asleep or staying asleep on a regular basis.
Women are significantly more likely to experience insomnia than men, especially during hormonal transitions such as pregnancy, perimenopause, and menopause.

Some surprising facts about sleep and health:
Poor sleep is strongly linked to increased inflammation and blood sugar instability — even one night of poor sleep can raise next-day insulin resistance.
People with chronic insomnia have a 2–3 times higher risk of developing depression and anxiety disorders.
Disrupted sleep can impair the brain’s ability to clear toxins, including beta-amyloid proteins associated with Alzheimer’s disease.
The gut-brain axis plays a major role — people with gut imbalances or irritable bowel syndrome often experience significantly worse sleep quality.
These statistics help explain why simply taking a sleeping pill rarely leads to lasting improvement. When sleep is off, it’s usually a signal that multiple systems in the body are out of balance — exactly the kind of interconnected problem functional medicine is designed to address.
Common Signs & Symptoms of Insomnia & Sleep Disorders
Insomnia and sleep disorders can show up in many different ways. You may recognize some — or all — of these patterns:
Difficulty falling asleep, even when you feel exhausted
Waking up multiple times during the night, especially between 2 and 4 AM
Jolting awake with a racing mind or sudden anxiety
Waking up too early and being unable to fall back asleep
Feeling like you’ve barely slept, even after 7–9 hours in bed
Waking up feeling unrefreshed, groggy, or more tired than when you went to bed
Daytime symptoms such as brain fog, irritability, low mood, trouble concentrating, or afternoon crashes
These symptoms often create a vicious cycle — the worse you sleep, the more your body struggles to regulate energy, mood, and hormones the next day.
Sleep issues rarely exist in isolation. When these patterns persist, they are usually signals that deeper imbalances need attention.

Common Root Causes of Chronic Insomnia
While every patient is unique, several key patterns frequently emerge when we investigate chronic insomnia:
Cortisol should be highest in the morning and lowest at night. In many insomnia sufferers, this natural rhythm is reversed or flattened.
Nighttime drops in blood sugar can trigger a surge of adrenaline and cortisol, causing sudden awakenings
Low progesterone, testosterone imbalance, perimenopause, and thyroid dysfunction commonly disrupt sleep architecture.
The gut plays a major role in producing serotonin and GABA — two neurotransmitters essential for calm, restorative sleep.
Chronic Stress & Nervous System Overactivation:
Persistent “fight or flight” activation keeps the brain from shifting into restorative sleep cycles.
Hidden Stressors (toxins):
Mold exposure, chronic infections, and toxin burden can all increase inflammatory signaling that disrupts sleep.
Sleep problems are often multi-factorial. This is exactly why simple fixes or sleeping pills rarely provide lasting relief — they don’t address the combination of issues driving the disruption.
Our Functional Medicine Approach to Restoring Sleep
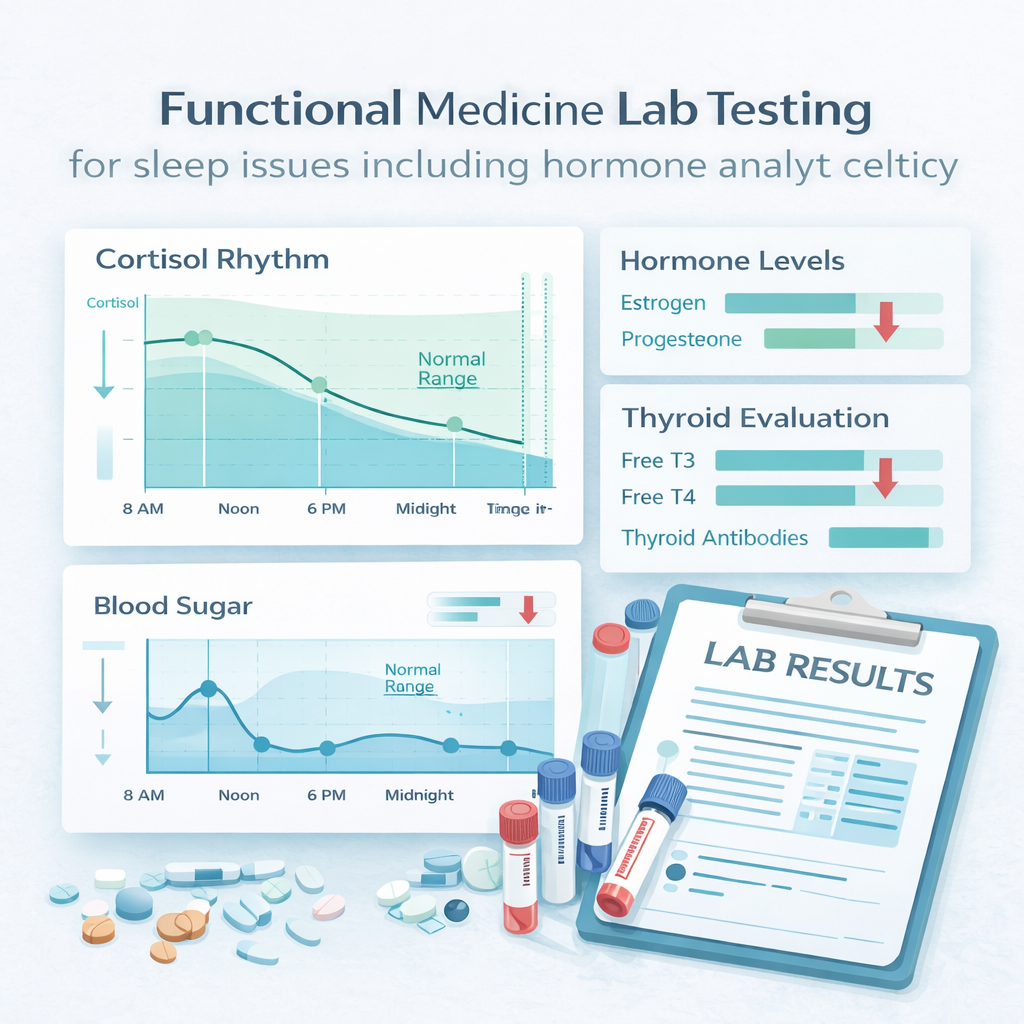
Sleep issues rarely have just one cause. That’s why the first step is understanding what’s happening beneath the surface. We use a combination of detailed health history and advanced testing when needed to evaluate:
Detailed symptom history and timeline
Cortisol rhythm testing
Comprehensive hormone analysis
Full thyroid evaluation beyond basic TSH
Blood sugar and metabolic assessment
Gut health evaluation
Nutrient status testing
Evaluation for environmental stressors when appropriate
We do not run standardized sleep panels.
Every test is chosen based on your history and symptom pattern.
Because sleep improves when physiology improves.
What Improves When Sleep Improves
Sleep is not passive. It is not simply “rest.” It is one of the most biologically active and restorative processes in the human body.
When the root cause of insomnia is addressed and sleep normalizes, improvements extend far beyond just feeling less tired.
Patients often experience:
More stable, consistent daytime energy
Reduced anxiety and nervous system reactivity
Improved mood and emotional resilience
Better stress tolerance
Fewer afternoon crashes
Improved weight regulation and metabolism
Reduced sugar cravings
More balanced hormones
Decreased inflammation
Improved digestion and gut function
Stronger immune resilience
But the benefits go even deeper.
During deep sleep:
Growth hormone is released to repair tissues
Muscles recover
Cells regenerate
The immune system recalibrates
Inflammation decreases
Hormones are regulated
Chronic sleep disruption impairs this repair process. Over time, this can contribute to accelerated aging, metabolic dysfunction, immune imbalance, and hormone dysregulation.


Sleep Is When the Brain Detoxifies
One of the most critical functions of sleep is brain detoxification.
During deep sleep, the glymphatic system activates — a specialized waste-clearance system in the brain that removes metabolic byproducts, inflammatory compounds, and neurotoxic debris accumulated during the day.
When sleep is fragmented or shortened:
Brain detox is impaired
Cognitive clarity declines
Mood regulation suffers
Neuroinflammation can increase
This is one reason chronic insomnia is associated with brain fog, memory issues, anxiety, and long-term neurologic risk.
Sleep literally clears the brain.
Sleep Regulates Hormones
Cortisol, melatonin, insulin, leptin, ghrelin, growth hormone, thyroid hormones, testosterone, and progesterone all depend on proper sleep architecture.
When sleep improves:
Cortisol rhythms stabilize
Blood sugar becomes more balanced
Appetite hormones normalize
Sex hormones regulate more efficiently
Thyroid conversion improves
This is why sleep restoration often improves weight regulation, mood, libido, and metabolic function — even before other interventions are intensified.

Sleep Lowers Inflammation
Chronic insomnia increases inflammatory signaling throughout the body.
Elevated inflammation is linked to:
Autoimmune activation
Digestive disorders
Cardiovascular risk
Joint pain
Hormone disruption
When sleep stabilizes, inflammatory markers often decline naturally — because the body is finally allowed to recover.
Sleep Is Foundational!
You cannot fully optimize hormones, gut health, immune balance, detoxification, or metabolic function without addressing sleep. It is foundational physiology. When sleep stabilizes, the body shifts out of survival mode and into repair mode. And when the body is allowed to repair, healing becomes possible.
Who This Is For? = Everyone!
This approach may be right for you if:
You wake up at 2–4am consistently
You feel “tired but wired”
You’ve tried multiple supplements or medications
You’ve been told your labs are normal
You suspect stress, hormones, thyroid, or gut health are involved
You are looking for answers — not just sedation
It may not be ideal for those looking only for a prescription solution.

Ready to Break the Cycle?
If you are tired of cycling through temporary solutions and ready to understand what is actually disrupting your sleep,
we can help.
Sleep is not random. It is regulated physiology.
When the underlying systems are restored, natural sleep often returns.
Your Questions, Answered
-
It really depends on the underlying root causes and how consistently those factors are being addressed. Many patients begin to notice early improvements within a few weeks, but it’s common to have some ups and downs along the way. More meaningful, lasting changes typically develop over 6–12 weeks as we work deeper into the root causes and support the body’s natural rhythms. Long-term improvement comes from consistent, ongoing work to restore balance, not just quick fixes.
-
No. We work with you and your doctor to safely reduce or eliminate sleep medications ONLY when your body is ready and sleeping more naturally.
-
We commonly use salivary or urine cortisol testing, comprehensive hormone panels, gut health testing, and blood sugar assessments to uncover hidden imbalances. This type of testing is looking at different root causes.
-
Waking up around 2–4AM is common and usually not random.
It’s often a sign that something in your body is out of balance.
The most common causes include:
Blood sugar drops, which trigger stress hormones and wake you up
Cortisol imbalance, causing your body to feel alert at night
Hormonal changes, especially during perimenopause or menopause
Chronic stress, keeping your body in a “fight-or-flight” state
If this happens regularly, it’s usually a clue that your sleep issue has an underlying cause—not just a sleep problem.
-
Several nutrient deficiencies can contribute to poor sleep, including:
Magnesium
B vitamins
Vitamin D
These nutrients play a role in nervous system regulation and the production of sleep-related hormones like melatonin.
