Functional Medicine for
Mast Cell Activation Syndrome (MCAS)
Why MCAS Symptoms Persist Without a Root-Cause Approach

Living with Mast Cell Activation Syndrome (MCAS) often feels like your body is stuck in a constant state of high alert. Everyday triggers—foods, scents, temperature shifts, or even minor stress—can spark unpredictable episodes of flushing, digestive distress, brain fog, fatigue, or heart palpitations. Many people search for answers for years because conventional approaches often focus only on managing surface-level reactions rather than addressing why mast cells are overreacting in the first place.
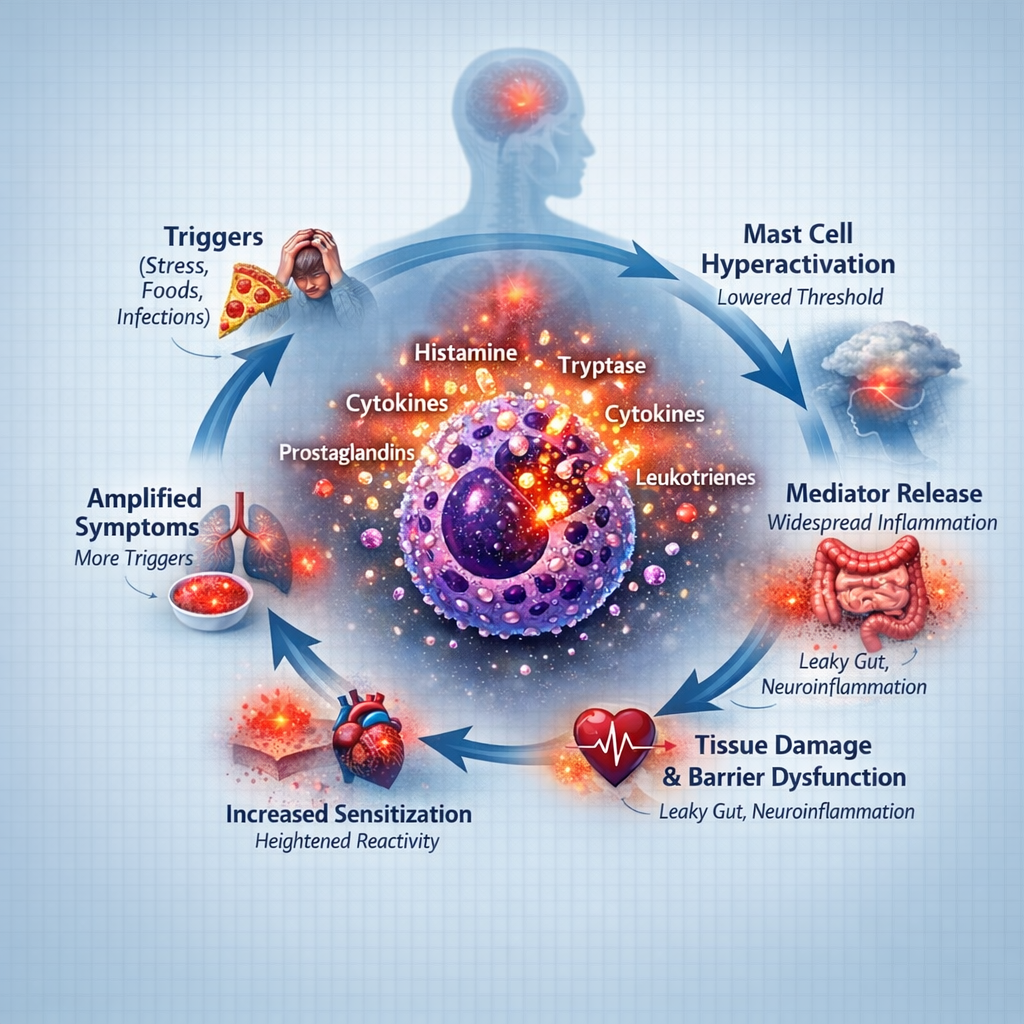
Mast Cell Activation Syndrome (MCAS) is a complex condition that can affect multiple systems throughout the body, often leading to a wide range of symptoms that may seem unrelated or difficult to explain. Mast cells are a key part of the immune system and play an important role in protecting the body. However, in MCAS, these cells can become overactive or dysregulated, releasing chemical mediators such as histamine inappropriately. This can trigger symptoms affecting the skin, digestive system, respiratory system, and nervous system.
At Premier Integrative Functional Medicine in Southern California, we take a comprehensive, root-cause approach to MCAS. By investigating underlying factors such as gut imbalances, environmental exposures, chronic stress, and genetic influences, we support your body’s natural ability to restore balance and resilience. If you’re tired of cycles that never seem to resolve, this page explains how functional medicine for Mast Cell Activation Syndrome can provide a clearer path forward.
MCAS Statistics and Surprising Facts – More Common Than Many Realize
Mast Cell Activation Syndrome affects far more people than previously understood, yet it remains under-recognized in conventional settings.
Estimates suggest MCAS may impact up to 4–17% of the population in certain studies, with a strong female predominance (approximately 4–5 times more common in women).
In patients evaluated for suspected mast cell disorders, confirmed idiopathic MCAS appears in roughly 4.4% overall, rising significantly among those with unexplained anaphylaxis-like episodes.
MCAS frequently overlaps with other conditions; research shows it in up to 31% of individuals who also have postural orthostatic tachycardia syndrome (POTS) and Ehlers-Danlos syndrome (EDS), compared to just 2% in those without this combination—often called the “trifecta.”
MCAS is often misidentified for years as IBS, fibromyalgia, chronic fatigue syndrome, or anxiety disorders because symptoms can migrate across body systems.
Mast cells are ancient immune “first responders” that evolved over hundreds of millions of years—when they become hyper-vigilant, even non-threatening signals can trigger widespread reactions.
Familial patterns are common; genetic predispositions can make mast cells more reactive, though environment and lifestyle play major amplifying roles.
The gut houses a large portion of the body’s mast cells, which explains why digestive issues and food sensitivities frequently appear alongside other MCAS patterns.
Mast cells don’t just play a role in allergic reactions—they are also closely connected to the nervous system. Mast cells can interact directly with nerve cells, which may help explain why many people with MCAS experience symptoms such as anxiety, brain fog, headaches, and heightened sensitivity to stress.
Common Signs and Symptoms of Mast Cell Activation Syndrome
Because mast cells reside throughout the body, MCAS symptoms can appear in nearly any system and often shift in unpredictable ways.
Skin-Related Symptoms
Sudden flushing or redness
Skin sensitivity
Itching, hives, or rashes
Swelling (angioedema)
Dermographism (skin writing when scratched)
Abdominal pain or cramping
Bloating, diarrhea, or nausea
Reflux or alternating bowel patterns
Food sensitivities
Respiratory Symptoms
Shortness of breath
Wheezing
Cardiovascular & Autonomic Symptoms
Rapid heart rate or palpitations
Blood pressure fluctuations
Lightheadedness or near-fainting
Neurological Symptoms
Brain fog or cognitive changes
Headaches
Fatigue, anxiety-like feelings, or insomnia
Dizziness or lightheadedness
Other Frequent Patterns
Temperature intolerance or chemical sensitivities
Widespread aches or joint discomfort
Episodes that resemble allergic reactions without a clear external trigger
Because symptoms can vary and overlap with other conditions, identifying underlying contributors is essential.
Why MCAS Symptoms Persist
Many individuals with MCAS find that symptoms continue despite trying multiple approaches. This is often because the underlying drivers of mast cell activation have not been fully addressed.
Mast cells are highly responsive to signals from different systems in the body, including the immune system, gut, and nervous system. When these systems are out of balance, mast cells can remain in a state of heightened reactivity. Factors such as chronic inflammation, gut microbiome imbalances, and ongoing environmental exposures may contribute to this persistent activation. In addition, stress and nervous system dysregulation can further amplify immune responses, making symptoms more unpredictable.
For some individuals, histamine imbalance also plays a role, particularly if the body has difficulty breaking down histamine efficiently. Nutrient deficiencies may further impact these processes, as certain vitamins and minerals are involved in immune regulation and histamine metabolism.
Because these factors often overlap and interact with one another, addressing only one area may not be enough. A more comprehensive approach that looks at the full picture is often needed to support better balance.
What Is Histamine Intolerance?
Histamine intolerance occurs when the body is unable to properly break down histamine, a naturally occurring compound involved in immune responses, digestion, and nervous system signaling.
Histamine is found in certain foods and is also released by mast cells as part of the immune response. Under normal conditions, enzymes such as diamine oxidase (DAO) help break down histamine in the body. However, when histamine breakdown is impaired or histamine levels become excessive, symptoms can develop.
These symptoms may include:
Headaches or migraines
Flushing or skin redness
Hives or itching
Digestive issues (bloating, diarrhea)
Nasal congestion
Rapid heart rate
Histamine intolerance is not the same as an allergy. Instead, it is often related to an imbalance between histamine intake, production, and breakdown. Factors such as gut health, nutrient status, and enzyme function can all influence how well the body processes histamine.
Feature
Primary Issue
Main Mechanism
Scope of Symptoms
Histamine Role
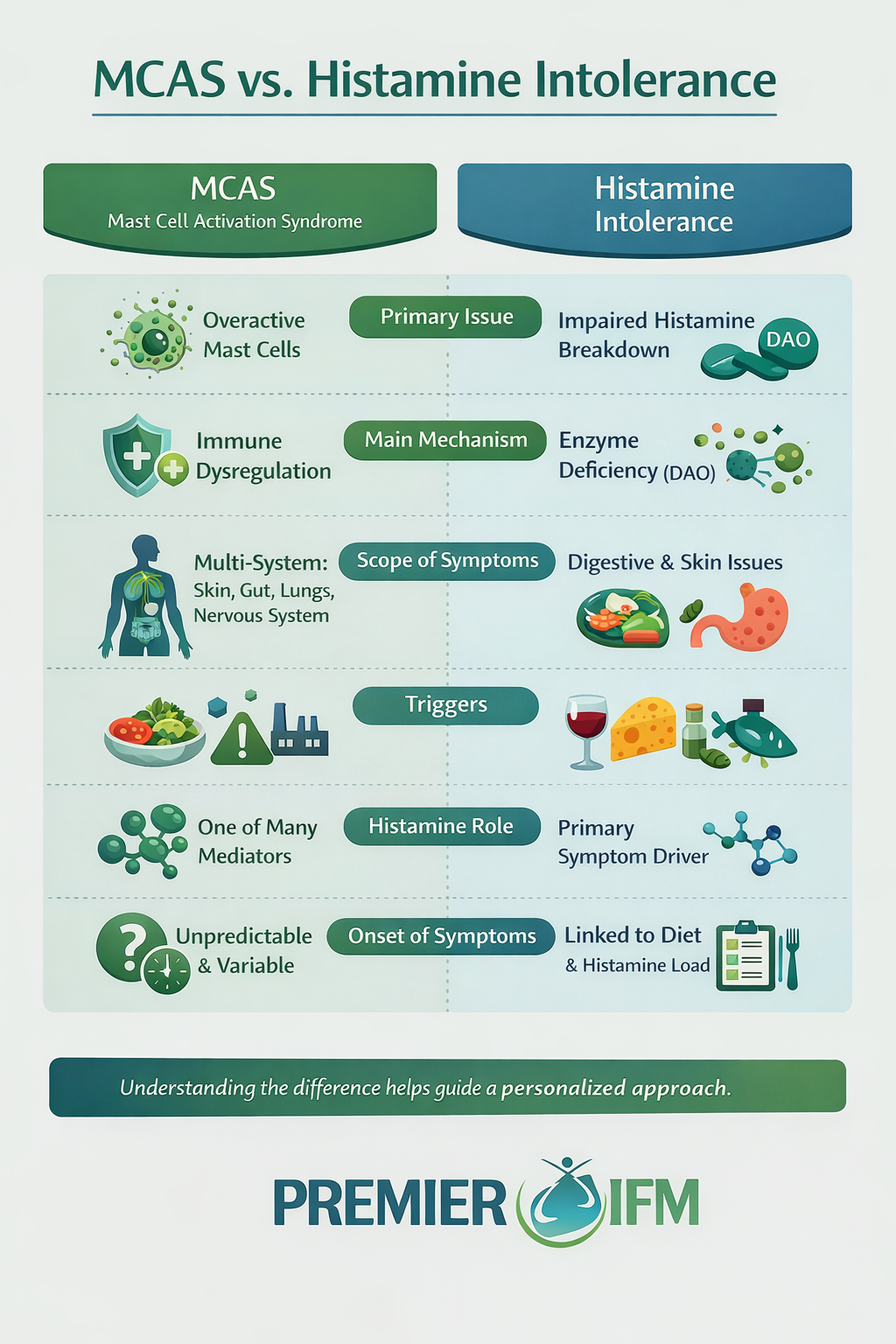
MCAS vs Histamine Intolerance
MCAS (Mast Cell Activation Syndrome)
Multi-system (skin, gut, lungs, nervous system)
Food, stress, temperature, environment, chemicals
Histamine Intolerance
Overactive mast cells releasing mediators (including histamine)
Impaired breakdown of histamine
Enzyme deficiency (often DAO)
Triggers
Onset of Symptoms
Underlying Factors
Immune system dysregulation
Histamine is one of many mediators released
Can be unpredictable and vary widely
Immune dysregulation, inflammation, gut issues, stress
High-histamine foods or reduced enzyme activity
High-histamine foods or reduced enzyme activity
Histamine is the primary driver of symptoms
Often linked to diet or cumulative histamine load
Gut health, nutrient deficiencies, enzymes function
Why This Distinction Matters
Although these conditions overlap, identifying whether symptoms are driven primarily by mast cell activation or histamine breakdown issues can help guide more effective strategies.
In many cases, individuals may experience features of both, especially when gut health, inflammation, and immune function are involved.

Why Functional Medicine & What It Can Do for MCAS
Functional medicine focuses on identifying the underlying factors that may be contributing to mast cell activation, rather than focusing only on symptom control.
Instead of asking:
👉 “How do we suppress symptoms?”
We ask:
👉 “What is driving mast cell activation in this individual?”
This approach allows for a more personalized understanding of symptoms and triggers.
At Premier Integrative & Functional Medicine, we take a comprehensive approach to understanding and supporting individuals with MCAS by examing interconnected areas that commonly influence mast cell behavior—such as gut microbiome imbalances, hidden environmental exposures (including mold), lingering infections, stress physiology, hormonal fluctuations, and genetic variations. Through personalized nutrition plans, lifestyle modifications, and targeted laboratory insights, we support the body’s innate ability to calm over-reactivity and build greater resilience.
The Functional Medicine Approach to MCAS
Our comprehensive approach to understanding and supporting individuals with MCAS includes:
Identifying Triggers and Patterns
Looking at:
Food-related triggers
Environmental exposures
Stress patterns
Lifestyle factors
Supporting Gut Health
Focusing on restoring balance within the microbiome and improving digestive function.
Reducing Immune System Overactivation
Addressing factors that may contribute to chronic immune stimulation.
Supporting Histamine Balance
Helping the body better regulate and process histamine through targeted strategies.
Personalized Care
Because MCAS presents differently in each individual, care is tailored to the person—not just the condition.

Frequently Asked Questions
-
MCAS is a condition in which mast cells release chemical mediators inappropriately, leading to symptoms affecting multiple systems in the body.
-
Mast cells respond to a wide range of triggers, including food, stress, environmental exposures, and internal imbalances, which can make symptoms vary from day to day.
-
Yes. Certain foods may contain or trigger the release of histamine, which can influence symptoms in some individuals.
-
No. Typical allergies usually involve a consistent, identifiable trigger. MCAS involves mast cells that can react to a wide range of internal or minor signals, leading to more variable and multi-system episodes.
-
Symptoms can overlap with many other conditions, and there is no single test that definitively identifies MCAS in all cases.
-
Symptoms fluctuate based on current stressors, diet, environment, sleep, and overall body burden. A root-cause approach helps lower this cumulative load.
-
Yes—certain genetic variations can increase mast cell reactivity, though lifestyle and environmental factors often determine how strongly those predispositions express.
More Light reading. Check out our related Blog posts
