Functional Medicine for Chronic Inflammation
Your Body Is Responding to Something
Why Inflammation Happens — And What It Means
Inflammation is a natural and essential part of the body’s defense system. When functioning properly, it helps protect against injury, infection, and harmful stimuli. Yes, inflammation is actually a good thing - when the body is in balance. However, when inflammation becomes chronic or persistent, it can contribute to a wide range of health issues.
Chronic inflammation is often described as a low-grade, ongoing immune response that may not produce obvious symptoms at first but can gradually affect multiple systems in the body.
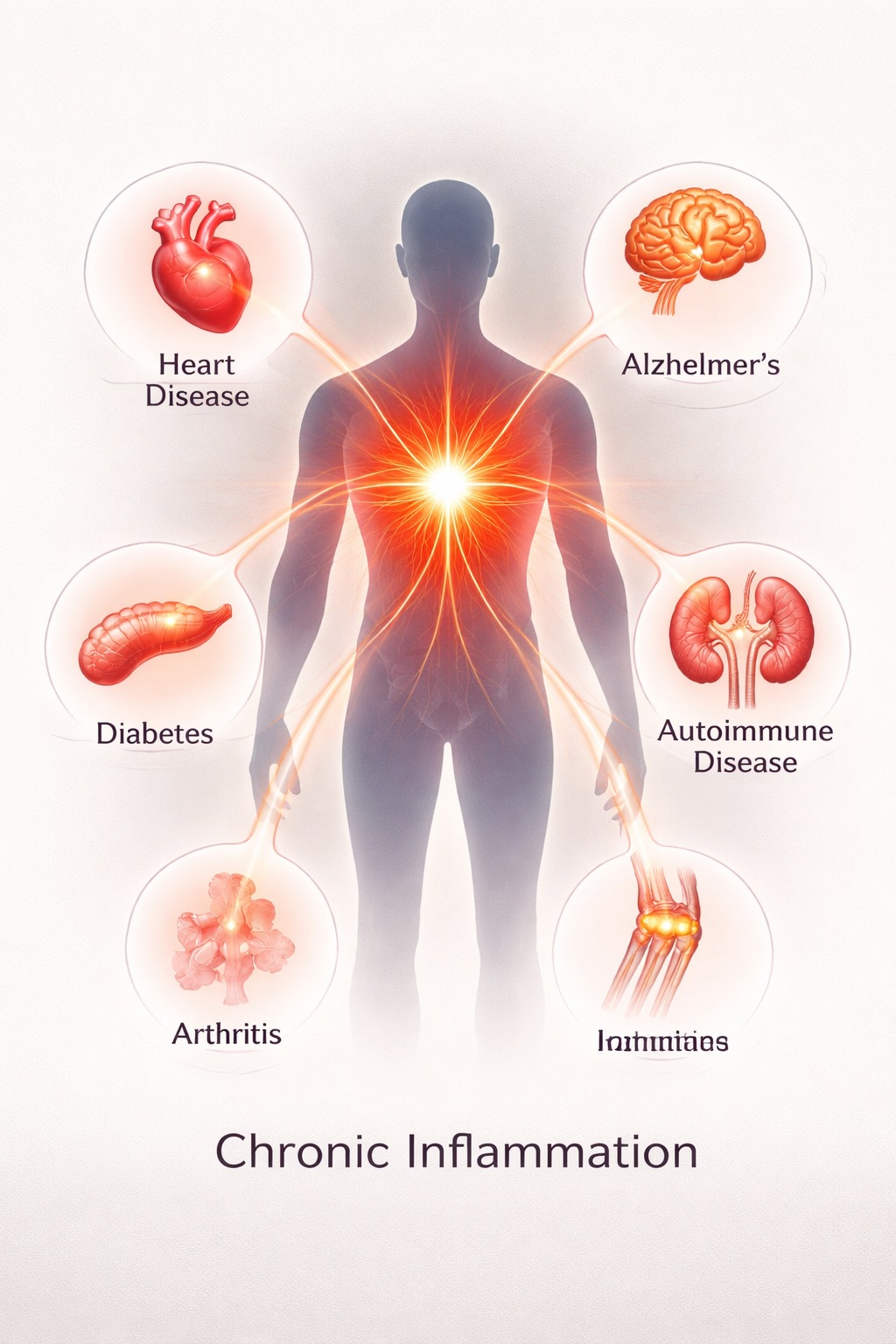
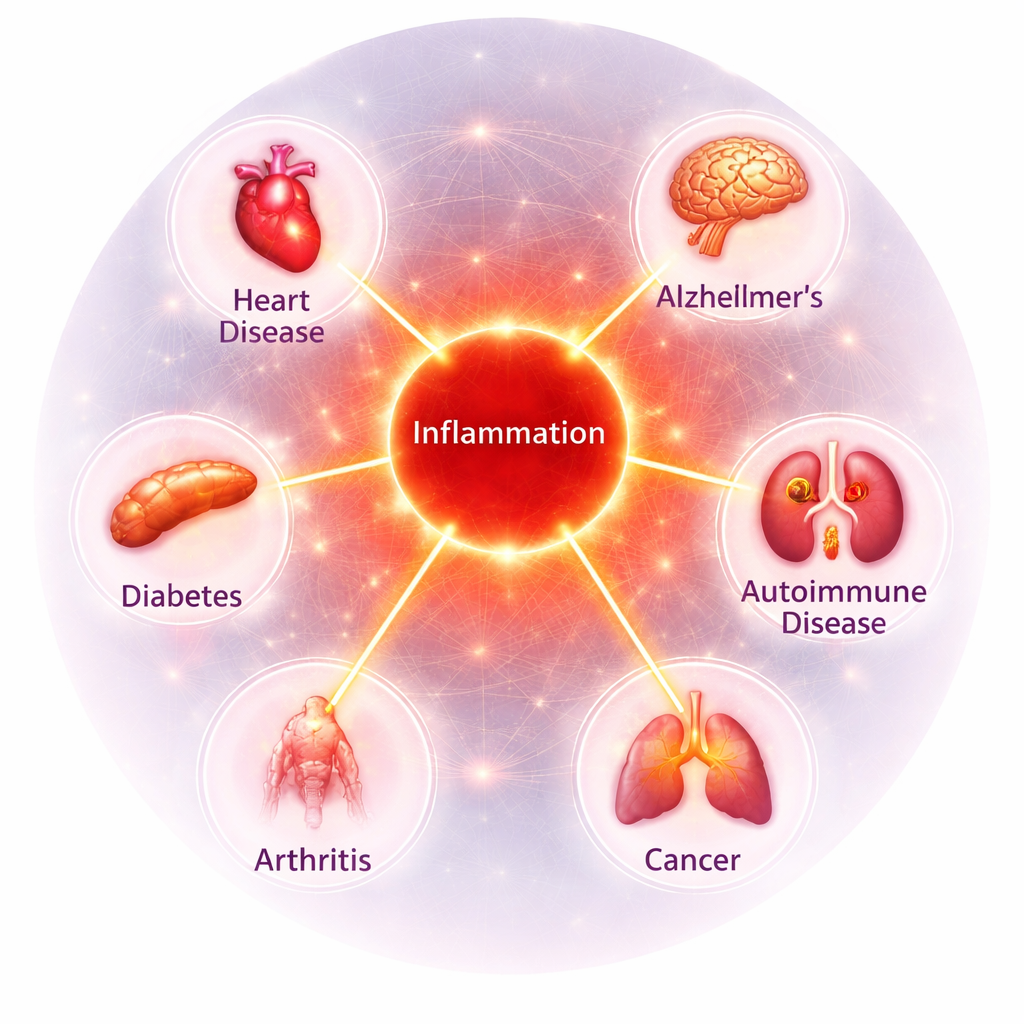
Research shows that chronic inflammation is associated with many common conditions, including:
Cardiovascular disease
Type 2 diabetes
Digestive conditions
Neurodegenerative diseases
At Premier Integrative & Functional Medicine, we view inflammation not as the root problem—but as a signal that something in the body needs attention. The goal is to identify and address the underlying triggers contributing to that response.
Chronic Inflammation: Prevalence and Impact
Chronic inflammation is increasingly recognized as a major contributor to disease.
According to the National Institutes of Health (NIH):
The Centers for Disease Control and Prevention (CDC) reports:
Additionally, research published in Nature Medicine has highlighted chronic inflammation as a common underlying factor in many modern health conditions.
These findings suggest that understanding and addressing inflammation may play an important role in long-term health.
Common Signs of Chronic Inflammation
Chronic inflammation can present in many different ways, depending on the systems involved.
Common symptoms may include:
Joint pain or stiffness
Digestive issues (bloating, discomfort)
Brain fog or difficulty concentrating
Frequent illness or slow recovery
Unexplained aches and pains
Because these symptoms are non-specific, identifying the underlying cause often requires a comprehensive evaluation.
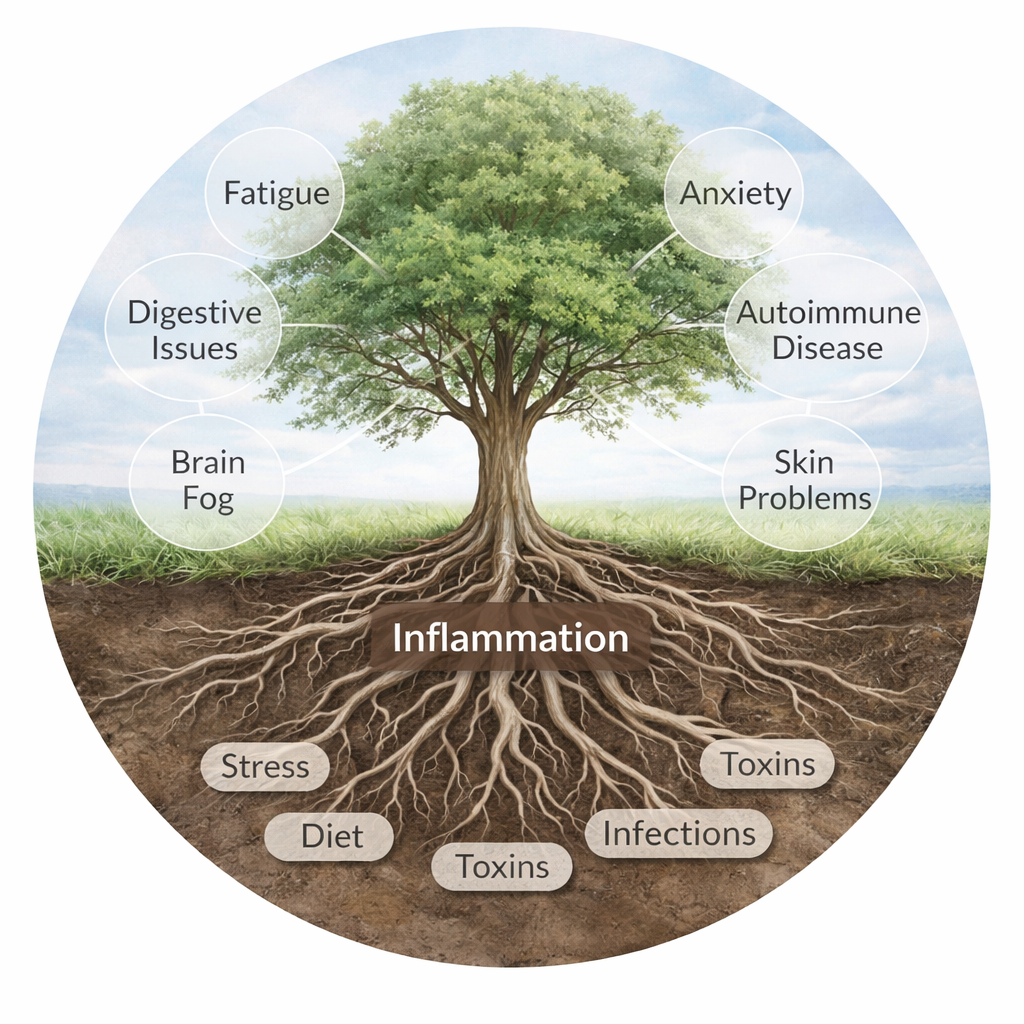
Why Inflammation Happens
Inflammation is not random—it is the body’s response to a perceived threat or imbalance. Several factors may contribute to chronic inflammation:
Diet and Blood Sugar Imbalance
Diets high in processed foods, refined sugars, and unhealthy fats may contribute to inflammatory responses.
Research shows that dietary patterns can influence inflammatory markers in the body.
Gut Health and the Microbiome
The gut plays a central role in immune regulation.
Studies have shown that imbalances in the gut microbiome may contribute to inflammation and immune dysregulation.
Chronic Stress
Stress activates hormonal pathways that influence immune function.
Research shows that chronic stress can contribute to increased inflammation in the body and disrupt normal immune function.
Sleep Disruption
Sleep is essential for regulating inflammation.
Research shows that chronic sleep deprivation can promote low-grade inflammation, which is linked to the development of metabolic and neurodegenerative conditions.
Environmental Exposures
Pollutants, toxins, and chemicals may contribute to inflammatory responses.
Research continues to explore how environmental exposures influence immune and inflammatory pathways.
Sedentary Lifestyle
Physical inactivity has been associated with increased inflammatory markers, while regular movement may help support healthy immune function.
Why Inflammation Matters in Functional Medicine
Functional medicine focuses on understanding why inflammation is occurring, rather than simply suppressing it.
Inflammation can be:
A response to infection
A reaction to food sensitivities
A result of gut imbalance
A signal of metabolic dysfunction
A response to chronic stress or environmental exposure
Rather than viewing inflammation as the problem itself, it is seen as a messenger indicating underlying imbalance.
The Functional Medicine Approach to Chronic Inflammation
At Premier Integrative & Functional Medicine, we take a personalized, root-cause approach to chronic inflammation—focusing on identifying why the inflammatory response is occurring in the first place.
Rather than simply trying to suppress inflammation, we work to uncover and address the underlying triggers that may be driving it. For many patients, inflammation is not the problem itself, but a signal that something deeper in the body needs attention.
Identifying the Root Causes
Chronic inflammation is often influenced by multiple factors. We evaluate for common contributors such as:
Gut imbalances and microbiome disruption
Food sensitivities or dietary triggers
Blood sugar instability
Chronic stress and nervous system dysregulation
Environmental exposures and toxins
Nutrient deficiencies
Supporting Anti-Inflammatory Pathways
Once underlying factors are identified, we focus on supporting the body’s natural ability to regulate inflammation through:
Targeted nutrition and anti-inflammatory dietary strategies
Stabilizing blood sugar and metabolic function
Restoring gut health and improving digestion
Supporting detoxification pathways when appropriate
Restoring Balance to the Immune System
Inflammation is closely tied to immune function. Our goal is not to “shut down” the immune system, but to help it function more appropriately and efficiently.
This may involve:
Reducing chronic immune activation
Supporting immune tolerance
Addressing triggers that keep the body in a state of ongoing response
Building Long-Term Resilience
Chronic inflammation often develops over time, and lasting improvement requires a sustainable approach. We help patients build long-term strategies that support overall health, including:
Stress management and nervous system support
Sleep optimization
Regular movement and physical activity
Lifestyle changes that reduce ongoing inflammatory triggers
A Personalized Approach
No two individuals experience inflammation the same way. Each care plan is tailored to the individual, based on their health history, symptoms, and underlying contributors.
By addressing the root causes of inflammation, the goal is to support the body’s ability to return to a more balanced and regulated state over time.

Frequently Asked Questions
Still have questions? Take a look at the FAQ or reach out anytime. If you’re feeling ready, go ahead and apply.
-
No. Acute inflammation is a normal and necessary response. Problems arise when inflammation becomes chronic or uncontrolled.
-
In many cases, addressing underlying factors such as diet, lifestyle, and environmental exposures may help reduce inflammation. - Although rewarding, it is a lot of work on the individuals part.
-
Inflammation can be assessed through markers such as:
C-reactive protein (CRP)
Erythrocyte sedimentation rate (ESR)
Homocysteine
Other laboratory markers
-
Yes. Dietary patterns have been shown to influence inflammatory processes in the body.
-
This varies depending on the individual, underlying causes, and if you are fighting it from all angles. Improvements may occur over time with consistent lifestyle and nutritional support.
